TeamstersCare provides its members with medical benefits through an HMO and an Out of Area Option:
Blue Care Network. Certificate of Coverage Blue Elect Plus for Small Groups. This Certificate of Coverage (Certificate) describes the Benefits provided to you and is a contract between you as an enrolled Member and Blue Care Network of Michigan (BCN). It includes General Provisions and Your Benefits. BLUE ELECT PLUS is a product of BCN, an. Blue Care Elect Preferred PPO. Home → Blue Care Elect Preferred PPO. Schedule of Benefits. This is the Schedule of Benefits that is a part of your Benefit Description. This chart describes the cost share amounts that you must pay for covered services. It also shows the.
- HMO Blue New England Option
- Blue Care Elect Preferred Out of Area Option
Whether you will participate in the HMO or Out of Area option will depend on where you live. The HMO Blue New England plan covers members who live in certain geographical service areas, including all cities and towns of Massachusetts, Rhode Island, Connecticut, Maine, New Hampshire and Vermont. If you are a TeamstersCare member living outside of New England, or a member with an eligible dependent living permanently outside of New England, you are covered by Blue Care Elect Preferred.
Both the HMO Blue and Out of Area Option cover a broad range of services, including:
- Doctor's care, including maternity, pediatric and well-child visits
- Hospital care (both in- and out-patient)
- Surgery and emergency care
- Diagnostic x-rays and laboratory tests
- Authorized services for rehab, acute care, home health and early intervention
- Chiropractic care, podiatry, nutrition and ambulatory transport
- Authorized medical equipment
HMO Blue New England Option
Your Primary Care Physician
When you enroll in HMO Blue New England, you and each family member must select an in-network primary care physician (PCP). Your PCP will direct and monitor your care, and will be the first person you call when you need routine or sick care. They will also guide you through any referrals you may need for specialized services.
Emergency Care
In an emergency, such as a suspected heart attack, stroke or poisoning, you should go directly to the nearest medical facility or dial 911 (or your local emergency phone number). You'll pay a $75 copayment for emergency room services, though this copay is waived if you're admitted to the hospital.
What Does Blue Care Insurance Cover
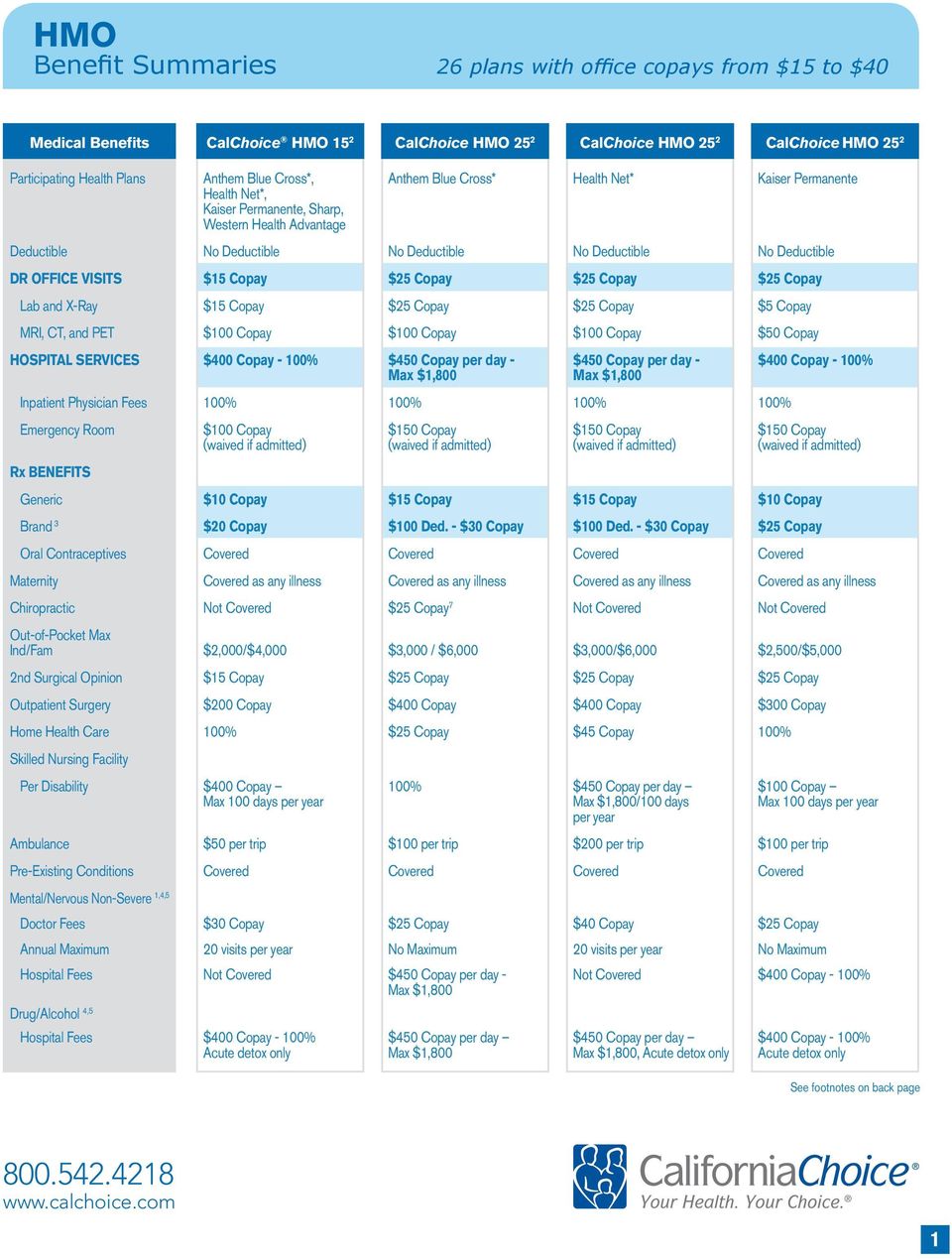
Basic Medical Benefits
*Check with HMO Blue New England for (1) limitations that might apply to services listed above or (2) coverage of any items not identified above.
Important Note: This summary is not meant to be a complete description of your TeamstersCare benefits. For eligibility related issues, or if you have any questions, call Charlestown Member Services.
Blue Care Elect Preferred Out of Area Option
As a Blue Care Elect Preferred Member, you are not required to select a Primary Care Physician (PCP). Instead, you and your dependents have two basic options for care: (1) you can take advantage of discounted services by using a Blue Care Elect Preferred Provider or (2) you can use a non-network provider.
If you use an in-network provider, the cost of most services (less any copayment) will be covered in full. If you use a non-network provider, most expenses are covered at 80% of reasonable and customary amounts after a $250 individual/$500 family deductible. The out-of-network co-insurance maximum is $1,000 per individual/$2,000 per family.
For more information on the Blue Care Elect Preferred Provider network, call 1-800-810-2583 or visit http://www.bluecrossma.com/nm/teamsters-care/.
Basic Medical Benefits
(1) of reasonable & customary expenses for covered charges. If the provider's actual charges are greater than the usual and customary charge, the member will be responsible for the applicable cost sharing amount based on the usual and customary fee, plus the difference between the usual and customary fee schedule and the provider's actual charges.
(2) one routine visit every five calendar years from age 19 through 29, one routine visit every three calendar years from age 30 through 39, one routine visit every two calendar years from age 40 to 54 and one routine visit per calendar year when age 55 or older.
(3) copay waived, if emergency room visit results in immediate hospitalization
Important Note: This summary is not meant to be a complete description of your TeamstersCare benefits. For a detailed listing of Blue Care Elect Preferred providers and facilities in your area, call 1-800-810-2583 or click here.
For more information on specific coverage under the Blue Care Elect Preferred option, claims-related questions, limitations that might apply to services listed above and coverage of any items not identified in this chart, call 1-800-241-0803.
Blue Cross Blue Shield Behavioral Health Benefit
Your Blue Cross Blue Shield medical benefit includes counseling and treatment for emotional difficulties, mental illness, substance abuse, family and marital problems and childhood concerns. You also have access to a variety of programs and services to help with chronic behavioral conditions.
Blue Care Elect Preferred 80 With Copay Center

To access outpatient behavioral health services, you simply make an appointment with an in-network provider and pay a $15 copay at the time of your visit. No referral or pre-authorization is necessary.
For new episodes of outpatient care, the first 12 visits are automatically authorized. If more than 12 visits are needed, your in-network provider will contact Blue Cross Blue Shield for additional authorizations on your behalf.
If you or your dependents have questions, you may call the Blue Cross Behavioral Health Coordination line at 1-800-444-2426 or go to http://www.bluecrossma.com/nm/teamsters-care/.
Important Note: As a TeamstersCare member, you also have access to behavioral health services through our in-house Employee Assistance Program.
Schedule of Benefits
This is the Schedule of Benefits that is a part of your Benefit Description. This chart describes the cost share amounts that you must pay for covered services. It also shows the benefit limits that apply for covered services. Do not rely on this chart alone. Be sure to read all parts of your Benefit Description to understand the requirements that you must follow to receive all of your coverage. You should also read the descriptions of covered services and the limitations and exclusions that apply for this coverage. These provisions are fully described in your Benefit Description. To be sure that you receive in-network benefits, yo must obtain all of your health care services and supplies from covered providers who participate in your PPO health care network. If you obtain covered services from a covered provider who does not participate in your PPO health care network, you will usually receive out-of-network benefits. Also, when it is required for coverage, you must receive an approval from Blue Cross and Blue Shield as outlined in your Benefit Description (see part 4). If an approval is required, you should make sure that you have received the approval from Blue Cross and Blue Shield before you receive the covered services. Otherwise you may have to pay all costs.
IMPORTANT NOTE: Blue Cross and Blue Shield and/or your group may change the provisions described in this Schedule of Benefits. If this is the case, the change is described in a rider. Be sure to read each rider (if there is any) that applies to your coverage in this health plan to see if it changes this Schedule of Benefits.
| Overall Member Cost Share Provisions | PCP/Plan Approved Benefits | Self-Referred Benefits |
| Deductible Your deductible per Calendar Year: This deductible applies to all self-referred benefits except for certain covered services as noted in this chart. | $0 | $500 per member $1,000 per family |
| The family deductible can be met by eligible costs incurred by any combination of members enrolled under the same family plan. But, no one member will have to pay more than the per member deductible. | ||
| Out-of-Pocket Maximum Your out-of-pocket maximum per Calendar Year: This out-of-pocket maximum is a total of your deductible and coinsurance, only for self-referred benefits. You will still have to pay any costs not included in this out-of-pocket maximum. | None | $2,000 per member $4,000 per family |
| The family out-of-pocket maximum can be met by eligible costs incurred by any combination of members enrolled under the same family plan. But, no one member will have to pay more than the per member out-of-pocket maximum. | ||
| Overall Benefit Maximum | None | None |
*Check with HMO Blue New England for (1) limitations that might apply to services listed above or (2) coverage of any items not identified above.
Important Note: This summary is not meant to be a complete description of your TeamstersCare benefits. For eligibility related issues, or if you have any questions, call Charlestown Member Services.
Blue Care Elect Preferred Out of Area Option
As a Blue Care Elect Preferred Member, you are not required to select a Primary Care Physician (PCP). Instead, you and your dependents have two basic options for care: (1) you can take advantage of discounted services by using a Blue Care Elect Preferred Provider or (2) you can use a non-network provider.
If you use an in-network provider, the cost of most services (less any copayment) will be covered in full. If you use a non-network provider, most expenses are covered at 80% of reasonable and customary amounts after a $250 individual/$500 family deductible. The out-of-network co-insurance maximum is $1,000 per individual/$2,000 per family.
For more information on the Blue Care Elect Preferred Provider network, call 1-800-810-2583 or visit http://www.bluecrossma.com/nm/teamsters-care/.
Basic Medical Benefits
(1) of reasonable & customary expenses for covered charges. If the provider's actual charges are greater than the usual and customary charge, the member will be responsible for the applicable cost sharing amount based on the usual and customary fee, plus the difference between the usual and customary fee schedule and the provider's actual charges.
(2) one routine visit every five calendar years from age 19 through 29, one routine visit every three calendar years from age 30 through 39, one routine visit every two calendar years from age 40 to 54 and one routine visit per calendar year when age 55 or older.
(3) copay waived, if emergency room visit results in immediate hospitalization
Important Note: This summary is not meant to be a complete description of your TeamstersCare benefits. For a detailed listing of Blue Care Elect Preferred providers and facilities in your area, call 1-800-810-2583 or click here.
For more information on specific coverage under the Blue Care Elect Preferred option, claims-related questions, limitations that might apply to services listed above and coverage of any items not identified in this chart, call 1-800-241-0803.
Blue Cross Blue Shield Behavioral Health Benefit
Your Blue Cross Blue Shield medical benefit includes counseling and treatment for emotional difficulties, mental illness, substance abuse, family and marital problems and childhood concerns. You also have access to a variety of programs and services to help with chronic behavioral conditions.
Blue Care Elect Preferred 80 With Copay Center
To access outpatient behavioral health services, you simply make an appointment with an in-network provider and pay a $15 copay at the time of your visit. No referral or pre-authorization is necessary.
For new episodes of outpatient care, the first 12 visits are automatically authorized. If more than 12 visits are needed, your in-network provider will contact Blue Cross Blue Shield for additional authorizations on your behalf.
If you or your dependents have questions, you may call the Blue Cross Behavioral Health Coordination line at 1-800-444-2426 or go to http://www.bluecrossma.com/nm/teamsters-care/.
Important Note: As a TeamstersCare member, you also have access to behavioral health services through our in-house Employee Assistance Program.
Schedule of Benefits
This is the Schedule of Benefits that is a part of your Benefit Description. This chart describes the cost share amounts that you must pay for covered services. It also shows the benefit limits that apply for covered services. Do not rely on this chart alone. Be sure to read all parts of your Benefit Description to understand the requirements that you must follow to receive all of your coverage. You should also read the descriptions of covered services and the limitations and exclusions that apply for this coverage. These provisions are fully described in your Benefit Description. To be sure that you receive in-network benefits, yo must obtain all of your health care services and supplies from covered providers who participate in your PPO health care network. If you obtain covered services from a covered provider who does not participate in your PPO health care network, you will usually receive out-of-network benefits. Also, when it is required for coverage, you must receive an approval from Blue Cross and Blue Shield as outlined in your Benefit Description (see part 4). If an approval is required, you should make sure that you have received the approval from Blue Cross and Blue Shield before you receive the covered services. Otherwise you may have to pay all costs.
IMPORTANT NOTE: Blue Cross and Blue Shield and/or your group may change the provisions described in this Schedule of Benefits. If this is the case, the change is described in a rider. Be sure to read each rider (if there is any) that applies to your coverage in this health plan to see if it changes this Schedule of Benefits.
| Overall Member Cost Share Provisions | PCP/Plan Approved Benefits | Self-Referred Benefits |
| Deductible Your deductible per Calendar Year: This deductible applies to all self-referred benefits except for certain covered services as noted in this chart. | $0 | $500 per member $1,000 per family |
| The family deductible can be met by eligible costs incurred by any combination of members enrolled under the same family plan. But, no one member will have to pay more than the per member deductible. | ||
| Out-of-Pocket Maximum Your out-of-pocket maximum per Calendar Year: This out-of-pocket maximum is a total of your deductible and coinsurance, only for self-referred benefits. You will still have to pay any costs not included in this out-of-pocket maximum. | None | $2,000 per member $4,000 per family |
| The family out-of-pocket maximum can be met by eligible costs incurred by any combination of members enrolled under the same family plan. But, no one member will have to pay more than the per member out-of-pocket maximum. | ||
| Overall Benefit Maximum | None | None |
| Covered Services | PCP/Plan Approved Benefits Your Cost Is: | Self-Referred Benefits Your Cost Is: |
| Admissions for Inpatient Medical and Surgical Care | ||
| In a General Hospital | $1,000 copayment per admission | 20% coinsurance after deductible |
| In a Chronic Disease Hospital | $1,000 copayment per admission | 20% coinsurance after deductible |
| In a Rehabilitation Hospital (60-day benefit limit per member per calendar year) | No charge up to benefit limit; then, you pay all costs | 20% coinsurance after deductible up to benefit limit; then, you pay all costs |
| In a Skilled Nursing Facility (100-day benefit limit per member per calendar year) | No charge up to benefit limit; then, you pay all costs | 20% coinsurance after deductible up to benefit limit; then, you pay all costs |
| Ambulance Services (ground or air ambulance transport) | ||
| Emergency Ambulance | No Charge | No charge (deductible does not apply) |
| Other Ambulance | No Charge | No charge (deductible does not apply) |
| Cardiac Rehabilitation | ||
| Outpatient Services | $20 copayment per visit | 20% coinsurance after deductible |
| Chiropractor Services (for members of any age) | ||
| Outpatient lab tests and x-rays | See Lab Tests, X-Rays, and Other Tests | See Lab Tests, X-Rays, and Other Tests |
| Outpatient medical care services, including spinal manipulation | $10 copayment per visit | 20% coinsurance after deductible |
| Dialysis Services | ||
| Outpatient services and home dialysis | No charge | 20% coinsurance after deductible |
| Durable Medical Equipment | ||
| Covered medical equipment rented or purchased for home use | 30% coinsurance | 50% coinsurance after deductible |
| One breast pump per birth (rented or purchased) | No charge | 50% coinsurance after deductible |
| No coverage is provided for hospital-grade breast pumps. | ||
| Early Intervention Services | ||
| (for an eligible child through age two) | No charge | No charge (deductible does not apply) |
| Emergency Medical Outpatient Services | ||
| Emergency room services | $100 copayment per visit | $100 copayment per visit (deductible does not apply) |
| The emergency room copayment is waived if the visit results in your being held for an overnight observation stay or being admitted for inpatient care within 24 hours. | ||
| Family or general practitioner, internist, pediatrician, geriatric specialist, audiologist, nurse practitioner, nurse midwife, podiatrist, optometrist, licensed dietician nutritionist, and multi-specialty provider group services | $20 copayment per visit | 20% coinsurance after deductible |
| Other covered provider services | $40 copayment per visit | 20% coinsurance after deductible |
| Hospital or health center services | $40 copayment per visit | 20% coinsurance after deductible |
| Home Health Care | ||
| Home care program | No charge | 20% coinsurance after deductible |
| Hospice Services | ||
| Inpatient or outpatient hospice services for terminally ill | No charge | 20% coinsurance after deductible |
| Infertility Services | ||
| Inpatient services | See Admissions for Inpatient Medical and Surgical Care | See Admissions for Inpatient Medical and Surgical Care |
| Outpatient surgical services | See Surgery as an Outpatient | See Surgery as an Outpatient |
| Outpatient lab tests and x-rays | See Lab Tests, X-Rays, and Other Tests | See Lab Tests, X-Rays, and Other Tests |
| Outpatient medical care services | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
| Lab Tests, X-Rays, and Other Tests | ||
| Outpatient Lab Tests | No charge | 20% coinsurance after deductible |
| Outpatient x-rays | No charge | 20% coinsurance after deductible |
| Outpatient CT scans, MRIs, and PET scans (copayment does not apply to interpretation costs) | $40 copayment per category of test per service date | 20% coinsurance after deductible |
| Other outpatient tests and preoperative tests | No Charge | 20% coinsurance after deductible |
| Maternity Services and Well Newborn Inpatient Care (includes $90/$45 for childbirth classes; deductible does not apply) | ||
| Maternity services (includes delivery and postnatal care) | $1,000 copayment per admission for inpatient hospital services, you pay nothing | 20% coinsurance after deductible |
| Prenatal Care | No Charge | 20% coinsurance after deductible |
| Well newborn care during enrolled mother's maternity admission | No Charge | 20% coinsurance (deductible does not apply) |
| Medical Care Outpatient Visits | ||
| Family or general practitioner, internist, pediatrician, geriatric specialist, audiologist, nurse practitioner, nurse midwife, podiatrist, optometrist, licensed dietician nutritionist, and multi-specialty provider group services | $20 copayment per visit | 20% coinsurance after deductible |
| Other covered provider services | $40 copayment per visit | 20% coinsurance after deductible |
| Hospital or health center services | $40 copayment per visit | 20% coinsurance after deductible |
| Medical Formulas (includes certain medical formulas and low protein foods) | ||
| $5,000 benefit limit per member per calendar year for low protein foods | No charge for covered services; otherwise you pay all costs | No charge (deductible does not apply) for covered services; otherwise, you pay all costs |
| Mental Health and Substance Abuse Treatment Refer to your Benefit Description for more information | ||
| Inpatient admissions in a General Hospital | $1,000 copayment per admission | 20% coinsurance after deductible |
| Inpatient admissions in a Mental Hospital or Substance Abuse Facility | $1,000 copayment per admission | 20% coinsurance after deductible |
| Outpatient services | $20 copayment per visit; or no charge for hospital services | 20% coinsurance after deductible |
| Oxygen and Respiratory Therapy | ||
| Oxygen and Equipment for its administration | No charge | 20% coinsurance after deductible |
| Outpatient respiratory therapy | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
| Podiatry Care | ||
| Outpatient lab tests and x-rays | See Lab Tests, X-Rays and Other Tests | See Lab Tests, X-Rays and Other Tests |
| Outpatient surgical services | See Surgery as an Outpatient | See Surgery as an Outpatient |
| Outpatient medical services | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
| Prescription Drugs and Supplies | ||
| Pharmacy Benefits | Not covered under this part of the group health plan | Not covered under this part of the group health plan |
| Preventive Health Care Services Includes: $150 Fitness Benefit $300 Weight Loss Program Benefit Refer to your Benefit Description for a complete description of covered services | ||
| Routine pediatric care (ten visits first year of life, three visits second year of life, two visits for age 2, and one visit per calendar year for age 3 through 18) | No charge for covered services; otherwise, you pay all costs | 20% coinsurance after deductible for covered services; otherwise, you pay all costs |
| These covered services include (but are not limited to): routine exams for age-based schedule; immunizations; routine lab tests and x-rays; and blood tests to screen for lead poisoning. | ||
| Preventive dental care | Not covered; you pay all costs | Not covered; you pay all costs |
| Routine adult exams and tests (one exam per member per calendar year) | No charge for covered services; otherwise, you pay all costs | 20% coinsurance after deductible for covered services; otherwise, you pay all costs |
| These covered services include (but are not limited to): routine exam per member per calendar year; immunizations; routine lab tests and x-rays; routine mammograms at least once between age 35 through 39 and once per calendar year for age 40 or older; blood tests to screen for lead poisoning; and routine colonoscopy every ten calendar years for a member age 50 or older. | ||
| Routine GYN exams (once per member per calendar year) | No charge for covered services; otherwise, you pay all costs | 20% coinsurance after deductible for covered services; otherwise you pay all costs |
| These covered services include a routine Pap smear test once per member per calendar year. | ||
| Family planning | No charge | 20% coinsurance after deductible |
| Routine hearing care services | Routine Hearing Exams/Tests: No charge Hearing Aids/Related Services: No charge for covered services; otherwise, you pay all costs | Routine Hearing Exams/Tests: 20% coinsurance after deductible Hearing Aids/Related Services: No charge (deductible does not apply) for covered services; otherwise, you pay all costs |
| These covered services include newborn hearing screening tests | ||
| This coverage is provided for $2,000 per member every 36 months. These covered services include: dispensing fees and acquisition costs; batteries; and repair of hearing aids. No benefits are provided for: replacement parts; charges to replace lost or broken hearing aids; and hearing aids delivered more than 60 days after termination date. | ||
| Routine vision exams | Not covered; you pay all costs | 20% coinsurance after deductible |
| Prosthetic Devices | ||
| Ostomy supplies | No charge | 20% coinsurance after deductible |
| Artificial limb devices (includes repairs) and other external prosthetics devices | No charge | 20% coinsurance after deductible |
| Radiation Therapy and Chemotherapy | ||
| Outpatient services | No charge | 20% coinsurance after deductible |
| Second Opinions | ||
| Outpatient second and third surgical opinions | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
| Short-term Rehabilitation Therapy | ||
| Outpatient physical, occupational, and speech therapy (100-visit benefit limit per member per calendar year) | $20 copayment per visit for covered services; otherwise you pay all costs | 20% coinsurance after deductible for covered services; otherwise you pay all costs |
| This benefit limit does not apply for: speech therapy; and when any of these covered services are furnished to treat autism spectrum disorders or as part of covered home health care. | ||
| Speech, Hearing and Language Disorder Treatment | ||
| Outpatient diagnostic tests | See Lab Tests, X-Rays, and Other Tests | See Lab Tests, X-Rays, and Other Tests |
| Outpatient speech therapy | See Short-Term Rehabilitation Therapy | See Short-Term Rehabilitation Therapy |
| Outpatient medical care services | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
| Surgery as an Outpatient (includes removal of impacted teeth that are fully or partially imbedded in the bone) | ||
| Surgical day care unit of hospital, ambulatory surgical facility, and hospital surgery services | $500 copayment per admission | 20% coinsurance after deductible |
| Sterilization procedure for a female member when performed as the primary procedure for family planning reasons | No charge | 20% coinsurance after deductible |
| Family or general practitioner, internist, pediatrician, geriatric specialist, audiologist, nurse practitioner, nurse midwife, podiatrist, optometrist, licensed dietician nutritionist, and multi-specialty provider group services | $20 copayment per office visit | 20% coinsurance after deductible |
| Other covered provider services (non-hospital) | $40 copayment per office visit | 20% coinsurance after deductible |
| Hospital or health center services | $40 copayment per visit | 20% coinsurance after deductible |
| TMJ Disorder Treatment | ||
| Outpatient x-rays | See Lab Tests, X-Rays, and Other Tests | See Lab Tests, X-Rays, and Other Tests |
| Outpatient surgical services | See Surgery as an Outpatient | See Surgery as an Outpatient |
| Outpatient physical therapy (short-term rehabilitation therapy benfit limit applies) | See Short-Term Rehabilitation Therapy | See Short-Term Rehabilitation Therapy |
| Outpatient medical care services | See Medical Care Outpatient Visits | See Medical Care Outpatient Visits |
Important Note about how your cost share amounts will be determined:
The cost share amount that you must pay will be determined by Blue Cross and Blue Shield based on the preferred provider's specialty type as shown on Blue Cross and Blue Shield's provider files at the time your claim is processed. A preferred provider may change his or her specialty at any time. However, Blue Cross and Blue Shield's provider files are updated with a new specialty type only once every three years. Until Blue Cross and Blue Shield's provider files are updated with a new specialty type for a preferred provider, the cost share amount that you pay will be based on the preferred provider's specialty type as shown on Blue Cross and Blue Shield's provider files.
Only one provider specialty type will be recognized. Some providers have primary and secondary provider specialty types. If you see a preferred provider for his or her secondary specialty, cost share amount that you must pay will be determined based on the preferred provider's primary specialty type. For example, a preferred provider is primarily a dermatologist but is also a 'family practitioner.' In this case, since this preferred provider's primary specialty type as shown on Blue Cross and Blue Shield's provider files is 'dermatologist,' you must pay the higher cost share amount.
Some physicians and other professional providers file claims through a facility. A provider specialty type cannot be identified when a preferred facility files a claim for payment. In this case, the cost share amount that you must pay as determined by Blue Cross and Blue Shield will be the higher cost share amount.
For preferred providers in other states, the local Blue Cross and/or Blue Shield Plan may have established provider specialty types that are not recognized by Blue Cross and Blue Shield. In those cases when a preferred provider's specialty type is not recognized, the cost share amount that you must pay as determined by Blue Cross and Blue Shield will be the higher cost share amount.

